
Do you have a Vestibular Migraine?
Vestibular migraine (VM) is a migraine attack accompanied by an episode of vertigo and dizziness. Approximately 30–50% of patients with migraine report vertigo, dizziness or balance disturbances with at least one migraine attack together (Neuhauser, Rasmussen).
The International Classification of Headache Disorders 3rd Edition (ICHD III) recognizes VM as an “episodic syndrome that may be associated with migraine”.
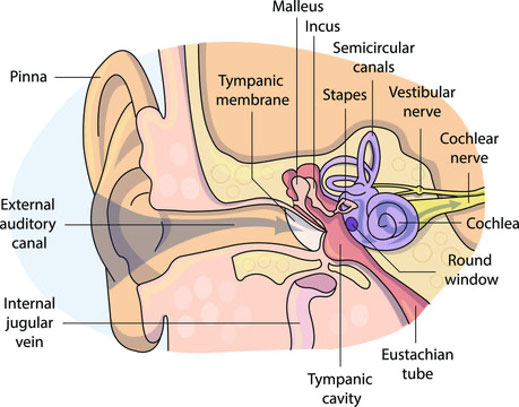
What is the vestibular system?
The vestibular system is essential for movement and equilibrium. This sensory system processes information about head position, spatial orientation and motion and sends it to the brain. The vestibular system (inner ear) coordinates movement between the eyes and head and provides important information about postural orientation.
Who gets a vestibular migraine?
Vestibular migraine can occur in any period of life (Dieterich M and Brandt). It presents more frequently in women than men with a gender ratio between 1.5 and 5 (Cass et al). In most patient’s vestibular migraine appears in an advanced period of life, and often with a temporal delay to the first onset of migraine (Neuhauser H, Leopold M, von Brevern M, et al). While people with standard migraine have a tendency to have motion sickness, those with VM are even more likely to suffer from motion sickness.
What are the symptoms of a vestibular migraine?
- Headaches
- Photophobia
- Phonophobia
- Aura
- Hearing / ear pain/ tinnitus
- Motion sickness
- Vertigo
- Dizziness
What triggers vestibular migraines?
- Insufficient or inconsistent sleep
- Excessive stress
- Menstruation
- Specific food
- Bright or scintillating lights
- Intense smells
- Intense noise
- Lack of exercise
- Screen time
- Complex patterns
How is Vestibular migraine diagnosed?
The International Classification of Headache Disorders 3rd Edition (ICHD III) recognizes VM as an “episodic syndrome that may be associated with migraine”.

Strategies to reduce symptoms:
Keep a diary – documentation can aid in the ability to succinctly and correctly diagnosis your migraine.
Exercise – Research has demonstrated exercise can be beneficial to decreasing the frequency and severity of migraine attacks. Starting slow is key, initially start by doing movement in a quiet room, this can reduce triggers such as lights and sound.
Sleep – There is lots of research showing how profoundly sleep can impact on migraine, too much and too little sleep can both be issues and for some people it is the sole trigger. Shift work and jet lag can impact massively. Try the following tips to see if they help:
- Go to bed and get up at the same time every day
- Spend some time outside every day, natural light helps fine tune our body clocks
- Sleep in an environment that is restful
- Do any exercises before your evening meal and not before bedtime
- Avoid caffeine and alcohol before bed
- If you are wide awake in the night don’t stay in bed
Diet – Stay well hydrated and eat at regular intervals though out the day.
Stress – Stress can be another big trigger to migraines. Strategies like, meditation, mindfulness, relaxing techniques are ways to manage stress, which can have a big impact on symptoms.
References:
Neuhauser HK, von Brevern M, Radtke A, et al. Epidemiology of vestibular vertigo: A neurotologic survey of the general population. Neurology 2005; 65(6): 898–904.
Rasmussen BK, Jensen R, Schroll M and Olesen J. Epidemiology of headache in a general population–A prevalence study. J Clin Epidemiol 1991; 44(11): 1147–1157
Dieterich M and Brandt T. Episodic vertigo related to migraine (90 cases): Vestibular migraine? J Neurol 1999; 246(10): 883–892.
Cass SP, Furman JM, Ankerstjerne K, et al. Migrainerelated vestibulopathy. Ann Otol Rhinol Laryngol 1997; 106(3): 182–189.
Neuhauser H, Leopold M, von Brevern M, et al. The interrelations of migraine, vertigo, and migrainous vertigo. Neurology 2001; 56(4): 436–441.
