Blood Flow Restriction Training
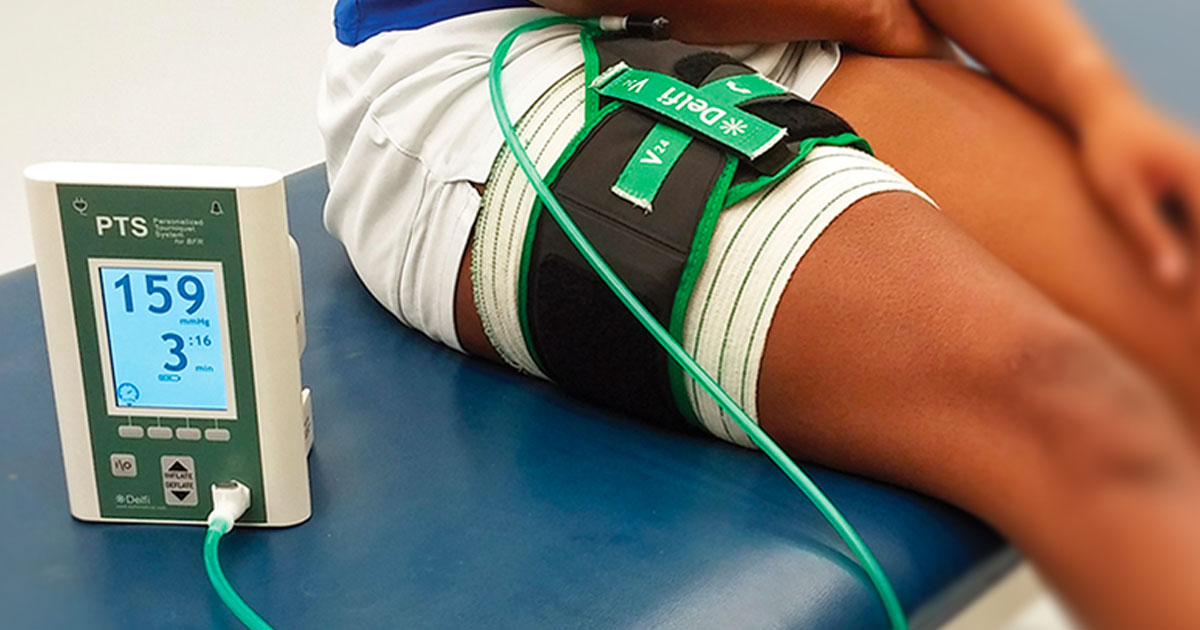
Blood Flow restriction, commonly referred to as BFR training, is a method whereby arterial inflow of the working muscles is partially restricted and venous outflow is completely obstructed to reduce the oxygen supply to the muscle (1). This type of training method was founded by the Japanese, and termed “kaatsu training” or “training with added pressure”(2). It can be used on either the upper or lower limb and is typically done with a tourniquet, but in the clinic setting a pressure cuff is commonly used.
Why does Blood Flow Restriction work for Strength Training?
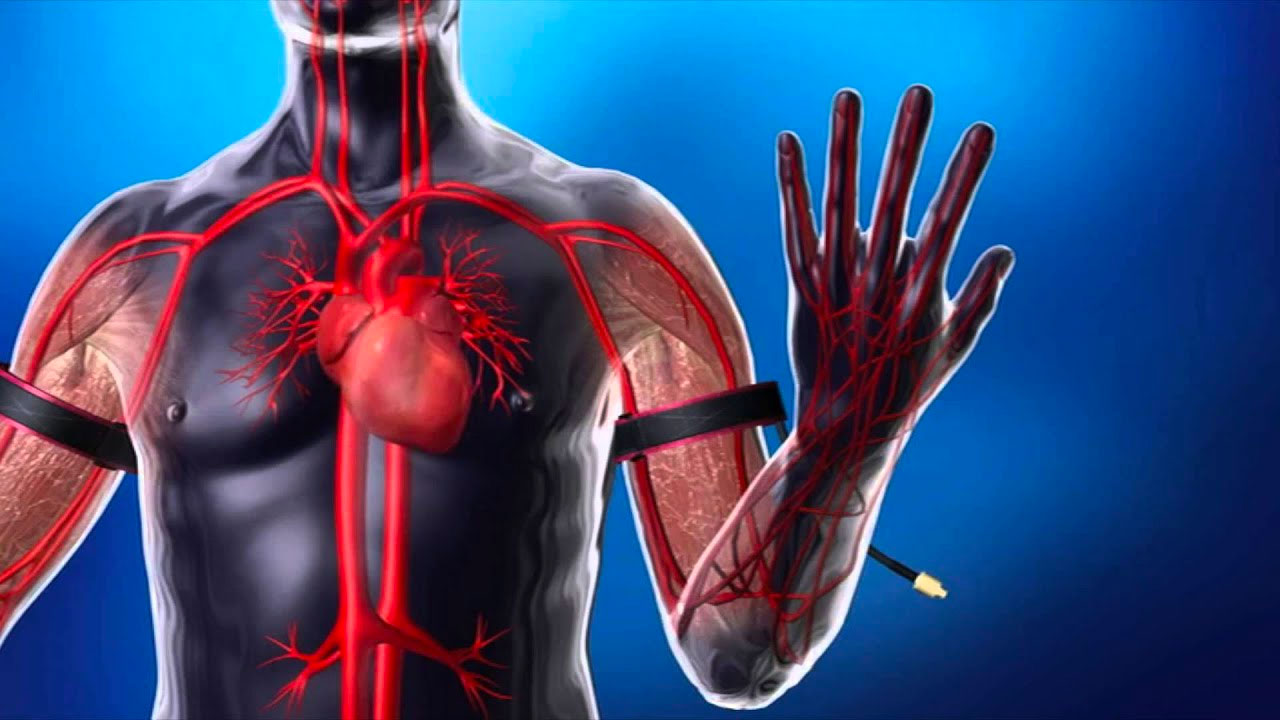
In resistance training, the compression of blood vessels causes a hypoxic environment within the muscle, meaning that the delivery of oxygen to the muscle is reduced. This increases the stress placed on the muscles, and subsequently causes the concentration of anabolic hormone levels to increase. Elevated anabolic hormones result in protein metabolism, which when combined with activation of these cells during training causes increased muscle hypertrophy (or growth).
A short duration program of low intensity training with BFR between 4-6 weeks has been proven to lead to 10-20% increase in muscle strength. This was a similar result to the group that performed high intensity exercise without BFR(3). In addition, they found that metabolic stress was increased with elevated blood lactate levels, leading to an increase in growth hormone and IGF-1 (anabolic protein)(4).
Generally, when trying to achieve strength gains, resistance will need to be set at 70% of 1RM whereas with BFR it’s only at 30%. This is why BFR training has been increasingly popular in the clinic as it can be used in ‘load compromised injuries’, when resistance must be restricted to aid the healing process of an injury.
Who is Blood Flow Restriction for?
Provided that you do not have any contraindications for BFR, (e.g. history of DVT, pregnancy, varicose veins and high blood pressure to name a few) there’s no reason BFR isn’t for you. However, the typical population that we will use it for in the clinic are:
- Post-operative lower limb injuries
- Patellofemoral pain syndrome
- Achilles or patella tendon
- Ankle syndesmosis injuries
- Deconditioned athletes who are unable to lift high volumes
What is involved in Blood Flow Restriction Training?
The cuff is inflated and placed as high as possible on the thigh or on the upper arm, and low intensity exercises are performed. This increases the water content of muscle cells and speeds up recruitment of fast-twitch muscle fibres.

Cuff Pressure
The pressure necessary to occlude venous return but still allow arteries to function is dependent upon the individual. However it is widely accepted that a wider cuff (10-20cm for lower limb) achieves the most even restriction.(5) There are 3 methods to determine cuff pressure:
- Standard pressure for everyone regardless of age, strength, size, etc.
- Pressure related to systolic blood pressure
- Pressure relative to thigh circumference
Overall it is accepted that the safest method that achieves the best results is to apply an individualised pressure. For example, an elderly individual and a body builder require different stimulus to improve strength, and therefore, require different pressure for BFR training(5). Generally, a perceived wrap tightness of 7 out of 10 results in optimal pressure, causing complete venous occlusion with partial arterial restriction(6).

Dosage
Like with any strength exercise an effective program required individualisation, especially in the athletic population. Not everyone will require the same amount of sets and repetitions. However, in a recent systematic review and meta-analysis (the gold standard in research)(7), a common range was: 4 sets of 30, 15, 15, 15 repetitions with a 1-minute rest between sets. The research found that higher repetition ranges (between 15 repetitions to fatigue) at only 30% of 1RM made greater enhancement for muscle gains.


Blood flow is an effective use of time to achieve maximal gains in load compromised athletes. Provided that there are no contraindications, as mentioned above, there really is no downside except increased fatigue from working harder!
References:
1. Scott B. R., Loenneke J. P., Slattery K. M., Dascombe B. J. (2015). Exercise with blood flow restriction: an updated evidence-based approach for enhanced muscular development. Sports Med.45 313–325. 10.1007/s40279-014-0288-1
2. Wernbom M., Augustsson J., Raastad T. (2008). Ischemic strength training: a low-load alternative to heavy resistance exercise? Scand. J. Med. Sci. Sports 18 401–416. 10.1111/j.1600-0838.2008.00788.x
3. Sousa, Jbc et al. (2016) Effects of strength training with blood flow restriction on torque, muscle activation and local muscular endurance in healthy subjects. Biology of sport vol. 34,1: 83-90
4. Patterson, S. D., Hughes, L., Warmington, S., Burr, J., Scott, B. R., Owens, J., Abe, T., Nielsen, J. L., Libardi, C. A., Laurentino, G., Neto, G. R., Brandner, C., Martin-Hernandez, J., & Loenneke, J. (2019). Blood Flow Restriction Exercise: Considerations of Methodology, Application, and Safety. Frontiers in physiology, 10, 533.
5. Bond CW, Hackney KJ, Brown SL, Noonan BC. (2019) Blood Flow Restriction Resistance Exercise as a Rehabilitation Modality Following Orthopaedic Surgery: A Review of Venous Thromboembolism Risk. Journal of Orthopaedic & Sports Physical Therapy. Jan;49(1):17-27.
6. Wilson J. M., Lowery R. P., Joy J. M., Loenneke J. P., Naimo M. A. (2013). Practical blood flow restriction training increases acute determinants of hypertrophy without increasing indices of muscle damage. J. Strength Cond. Res. 27 3068–3075.
7. Hughes L, Paton B, Rosenblatt B (2017). Blood flow restriction training in clinical musculoskeletal rehabilitation: a systematic review and meta-analysis. British Journal of Sports Medicine. Vol. 51 p1003-11
